kidney disease elderly dog
Chronic kidney disease
I'm Dr. Andrew Bentall, a kidney doctor at Mayo Clinic. I look after patients with kidney disease, either in the early stages, or with more advanced kidney disease considering dialysis and transplantation as treatment options. In this video, we'll cover the basics of chronic kidney disease. What is it? Who gets it? The symptoms, diagnosis and treatment. Whether you are looking for answers for yourself or for someone you love, we're here to give you the best information available.
Chronic kidney disease is a disease characterized by progressive damage and loss of function in the kidneys. It's estimated that chronic kidney disease affects about one in seven American adults. And most of those don't know they have it. Before we get into the disease itself, let's talk a little bit about the kidneys and what they do. Our kidneys play many important roles keeping our bodies in balance. They remove waste and toxins, excess water from the bloodstream, which is carried out of the body in urine. They helped to make hormones to produce red blood cells, and they turn vitamin D into its active form, so it's usable in the body.
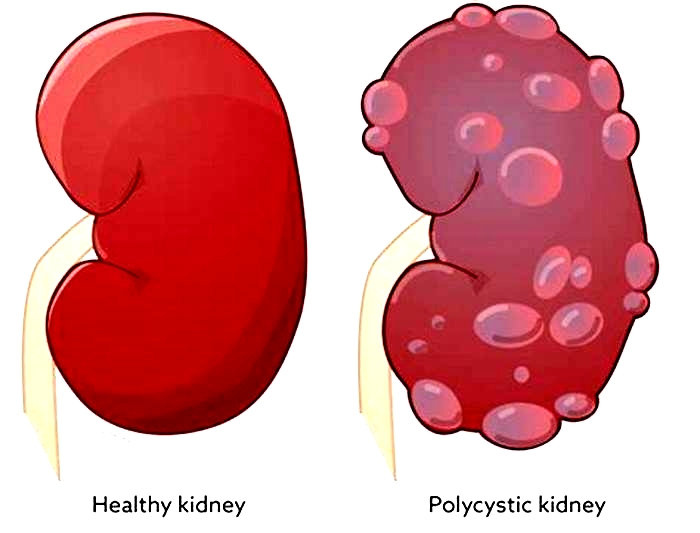
There are quite a few things that can cause or put you at higher risk for chronic kidney disease. Some of them are not things that can be avoided. Your risk is simply higher if you have a family history of certain genetic conditions like polycystic kidney disease or some autoimmune diseases like lupus or IgA nephropathy. Defects in the kidney structure can also cause your kidneys to fail, and you have an increased risk as you get older. Sometimes, other common medical conditions can increase your risk. Diabetes is the most common cause of kidney disease. Both type 1 and type 2 diabetes. But also heart disease and obesity can contribute to the damage that causes kidneys to fail. Urinary tract issues and inflammation in different parts of the kidney can also lead to long-term functional decline. There are things that are more under our control: Heavy or long-term use of certain medications, even those that are common over-the-counter. Smoking can also be a contributing factor to chronic kidney disease.
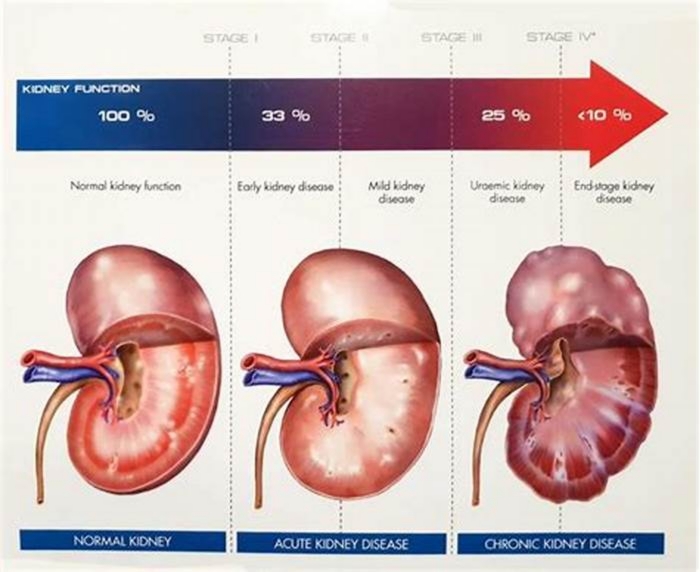
Often there are no outward signs in the earlier stages of chronic kidney disease, which is grouped into stages 1 through 5. Generally, earlier stages are known as 1 to 3. And as kidney disease progresses, you may notice the following symptoms. Nausea and vomiting, muscle cramps, loss of appetite, swelling via feet and ankles, dry, itchy skin, shortness of breath, trouble sleeping, urinating either too much or too little. However, these are usually in the later stages, but they can also happen in other disorders. So don't automatically interpret this as having kidney disease. But if you're experiencing anything that concerns you, you should make an appointment with your doctor.
Even before any symptoms appear, routine blood work can indicate that you might be in the early stages of chronic kidney disease. And the earlier it's detected, the easier it is to treat. This is why regular checkups with your doctor are important. If your doctor suspects the onset of chronic kidney disease, they may schedule a variety of other tests. They may also refer you to a kidney specialist, a nephrologist like myself. Urine tests can reveal abnormalities and give clues to the underlying cause of the chronic kidney disease. And this can also help to determine the underlying issues. Various imaging tests like ultrasounds or CT scans can be done to help your doctor assess the size, the structure, as well as evaluate the visible damage, inflammation or stones of your kidneys. And in some cases, a kidney biopsy may be necessary. And a small amount of tissue is taken with a needle and sent to the pathologist for further analysis.
Treatment is determined by what is causing your kidneys to not function normally. Treating the cause is key, leading to reduced complications and slowing progression of kidney disease. For example, getting better blood pressure control, improved sugar control and diabetes, and reducing weight are often key interventions. However, existing damage is not usually reversible. In some conditions, treatment can reverse the cause of the disease. So seeking medical review is really important. Individual complications vary, but treatment might include high blood pressure medication, diuretics to reduce fluid and swelling, supplements to relieve anemia, statins to lower cholesterol, or medications to protect your bones and prevent blood vessel calcification. A lower-protein diet may also be recommended. It reduces the amount of waste your kidneys need to filter from your blood. These can not only slow the damage of kidney disease, but make you feel better as well. When the damage has progressed to the point that 85 to 90 percent of your kidney function is gone, and they no longer work well enough to keep you alive, it's called end-stage kidney failure. But there are still options. There's dialysis, which uses a machine to filter the toxins and remove water from your body as your kidneys are no longer able to do this. Where possible, the preferred therapy is a kidney transplant. While an organ transplant can sound daunting, it's actually often the better alternative, and the closest thing to a cure, if you qualify for a kidney transplant.
If you have kidney disease, there are lifestyle choices. Namely quit smoking. Consuming alcohol in moderation. If you're overweight or obese, then try to lose weight. Staying active and getting exercise can help not only with your weight, but fatigue and stress. If your condition allows, keep up with your routine, whether that's working, hobbies, social activities, or other things you enjoy. It can be helpful to talk to someone you trust, a friend or relative who's good at listening. Or your doctor could also refer you to a therapist or social worker. It can also be helpful to find a support group and connect with people going through the same thing. Learning you have chronic kidney disease and learning how to live with it can be a challenge. But there are lots of ways to help you to be more comfortable for longer before more drastic measures are needed. And even then, there is plenty of hope. If you'd like to learn even more about chronic kidney disease, watch our other related videos or visit mayoclinic.org. We wish you well.
Chronic Renal Failure (CRF) in Dogs
What Is Chronic Renal Failure in Dogs?
Chronic renal failure (CRF), renal insufficiency, and chronic kidney disease (CKD) are all medical terms used to describe the same condition. It occurs when the kidneys are unable to perform their required tasks at the same level of efficiency as before.
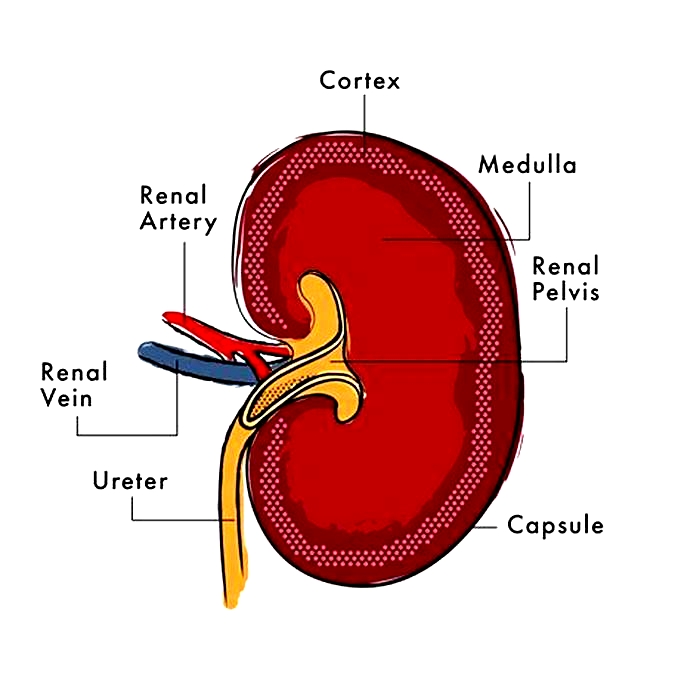
Dogs have two kidneys located on either side of their abdomen, that play a vital role in filtering waste from the body. Additionally, the kidneys serve to regulate fluid, mineral, and electrolyte balance; conserve water and protein; and play an important role in maintaining blood pressure and red blood cell production by making a hormone called erythropoietin.
Dogs cannot survive without their kidneys, and unfortunately, kidney transplants are yet to be a viable solution. Dialysis (a treatment for failing kidneys including the removal of waste) is often expensive and is extremely rare in dogs. However, early diagnosis and intervention is key to help maintain your dogs quality of life.
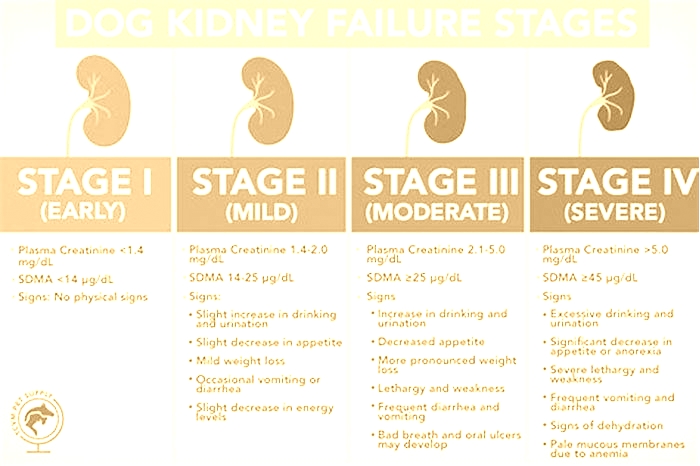
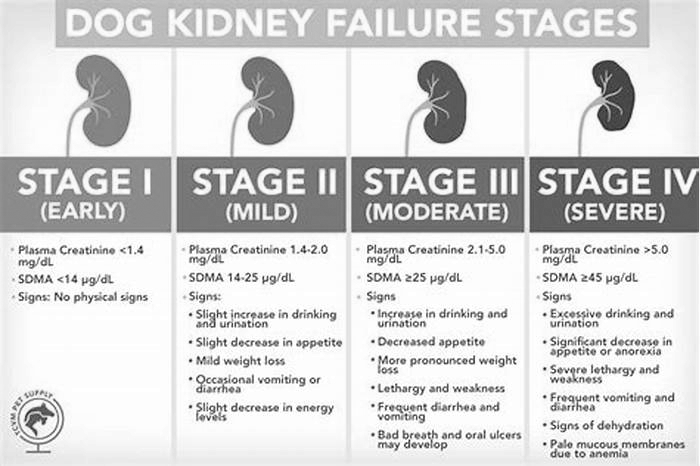
Once diagnosed, CRF is then classified into four different stages based on severity of clinical signs and laboratory values:
Stage I: Clinical signs usually not apparent
Stage II: Some clinical signs noted
Stage III: Many clinical signs noted, and pets often feel sick
Stage IV: Majority of clinical signs noted, pets often present as a crisis
Causes of Chronic Renal Failure in Dogs
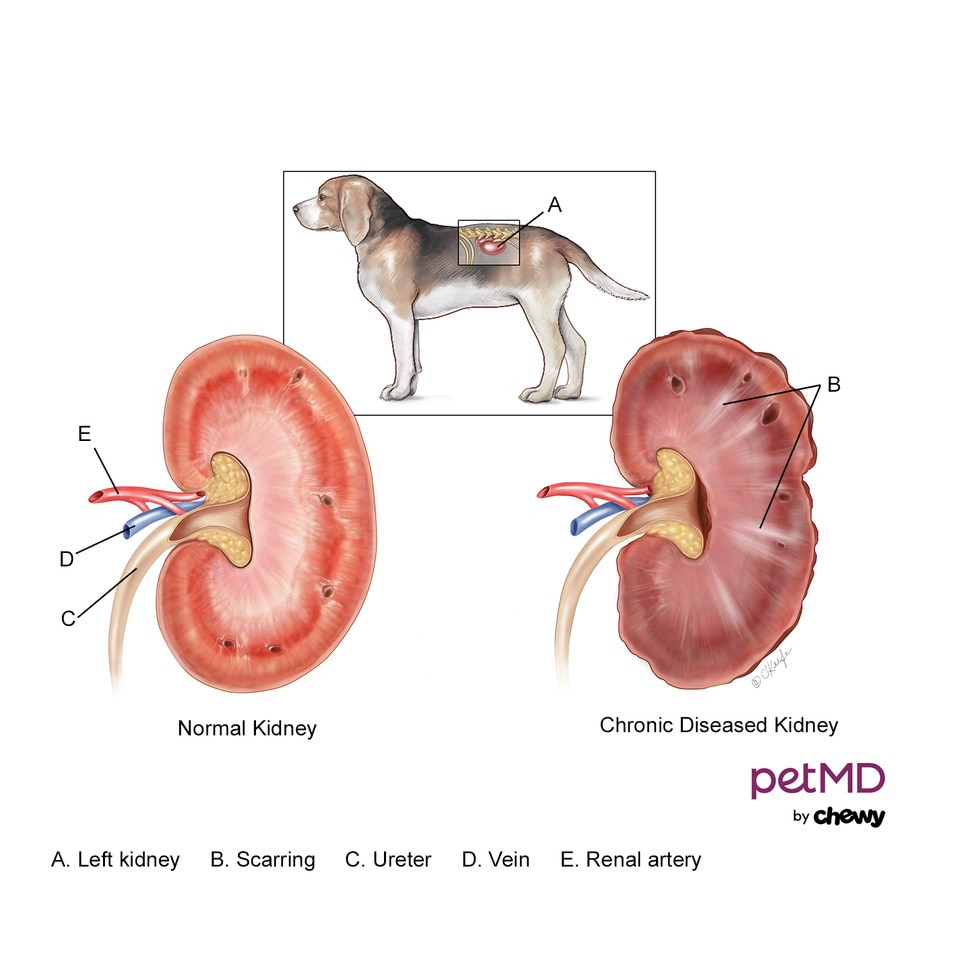
The term chronic in chronic renal failure means that the process has been ongoing, is progressive, and unfortunately, cannot be reversed. For some dogs, the disease could have occurred after a serious kidney injury such as from a severe infection (i.e., leptospirosis, pyelonephritis) or ingestion of a toxic substance such as anti-freeze, grapes, or raisins, and certain antibiotics.
For others, it could be inherited, such as with glomerular disease (a specific type of renal kidney disease) and amyloidosis (a rare organ disease) as seen in breeds like the Bernese Mountain Dog and Shar-pei.
For others, it could be attributed to underlying immune-mediated diseases, stroke-like events, or even from clotting disorders. In cases for newly diagnosed dogs the underlying cause will likely remain unknown.
Symptoms of Chronic Renal Failure in Dogs
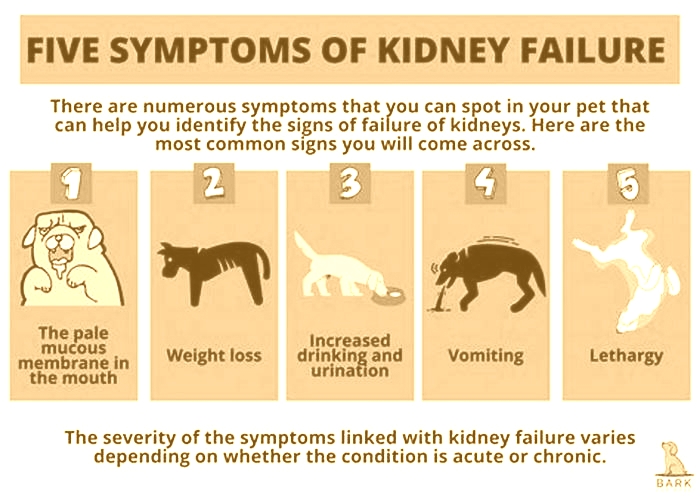
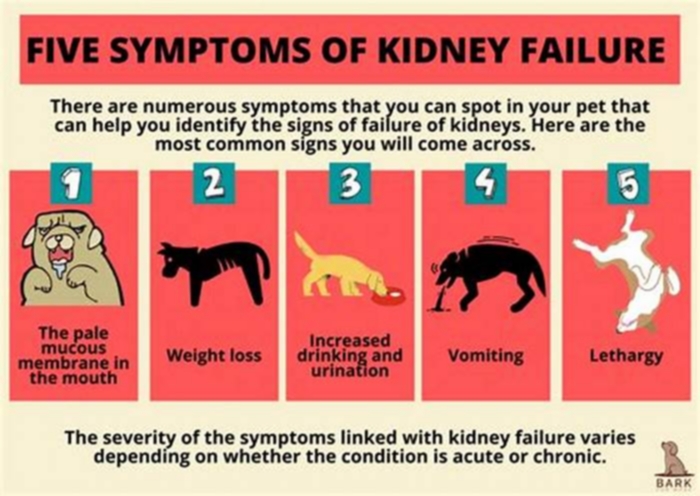
Clinical signs are often related to the severity of the CRF stage, meaning there are additional and more severe signs noted with stages III and IV than there are with stages I and II. Dogs often exhibit symptoms including:
Foul breath
Weight loss
Decreased appetite
Some dogs may show muscle wasting and signs attributed to high blood pressure, such as vision loss and weakness.
How Veterinarians Diagnose Chronic Renal Failure in Dogs
CRF is often diagnosed based on routine blood work and a urinalysis looking specifically at kidney markers such as:
Blood urea nitrogen (BUN): A by-product of protein metabolism, higher values can often indicate kidney failure
Creatinine (CREA): Measures how well kidneys are filtering waste from blood
Phosphorous: Elevated phosphorus levels typically indicate kidney damage
Electrolytes (Sodium, potassium, chloride)
Calcium
Red blood cell count: A low red blood cell count may indicate kidney failure
Symmetric dimethylarginine (SDMA): An additional test to help determine if kidney disease is present; it can be used for early detection of kidney disease
Urine specific gravity: A marker of how diluted or concentrated the urine is. Usually the higher the number, the more concentrated the urine is and the greater ability of the kidney to conserve water.
Your veterinarian will most likely recommend additional diagnostic testing, including:
A urine protein to creatinine (UPC) ratio to quantify how much protein is being lost in the urine
A urine culture, as dogs in CKD are more likely to acquire urinary tract infections
A blood pressure evaluation
Radiographs or abdominal ultrasound to screen for kidney stones or infarcts (areas of dead tissue)
Treatment of Chronic Renal Failure in Dogs
Dogs with CRF are generally older and have other ongoing issues, such as arthritis or liver disease, and so the management of CRF can be challenging. However, CRF can be managed, mostly with the aid of medications, diet, and hydration.
Specific management is geared toward each stage of the disease, with each progressive stage recommendations built upon the previous stage recommendations. Any dog in any stage with an increase in either UPC (urine protein to creatinine ratio) or high blood pressure will most likely be treated with medication.
Throughout your dogs life, any disease process or illness that could affect his hydration should be treated promptly with IV fluids. Other drugs will be prescribed based on the dogs diagnosis since renal metabolism will be affected and can lead to overdosages and/or worsening of the kidney disease.
Additionally, for all stages, fresh water should always be available, drinking should be encouraged, and adequate nutrition should be given daily. Dogs diagnosed with CRF are most likely prescribed a kidney friendly diet, which may include feeding your dog a canned diet of wet food that contains additional water.
Recovery and Prevention of Chronic Renal Failure in Dogs
As chronic renal failure is not curable and often progressive (although the timeline is variable) in nature, dogs diagnosed early on will benefit from nutritional management and consistent veterinary attention, which may include more frequent check-ups and blood work.
Dogs in stages I and II may often be monitored for further progression of signs, and some may be given a prescription diet specifically geared to help the kidney, by limiting the amount of work they must do.
Many dogs can go on to have a decent quality of life for many months to years. Dogs in stages III and IV often require more medical and dietary assistance. If secondary anemia is present, erythropoietin injections can be given at the direction of your veterinarian.
Dietary supplements, and phosphorus binders (to treat high phosphorus levels) may also be given for low potassium. Anti-nausea and anti-emetic (anti-vomiting) medications can also be prescribed for dogs with a poor appetite, vomiting, or nausea. Fluids given either intravenously or underneath the skin can help dehydration. Because of the severity of signs often seen in dogs with stage III and IV, and the amount of care and effort required to support these dogs, some may be humanely euthanized.
Chronic Renal Failure (CRF) In Dogs FAQs
How long can a dog live with kidney failure without treatment?
Left untreated, dogs in kidney failure will die, usually within a few days to a few weeks. Death is often preceded by loss of appetite, dehydration, weight loss, vomiting, and multi-organ failure.
Can dogs recover from chronic renal failure?
There is no cure for CRF. However, if CRF is caught early and managed correctly, most dogs that experience kidney disease can go on to live a relatively normal life with some changes and long-term management.
Can chronic renal failure in dogs be reversed?
While CRF is not reversible, early treatment can provide your pet with a happier, longer, and fuller life. Regular, semi-annual checkups are key to early diagnosis and treatment of the development of chronic renal disease.
Featured Image: iStock.com/Korneeva_Kristina
WRITTEN BY
Michael Kearley, DVMVeterinarian
Dr. Michael Kearley graduated from the University of Florida College of Veterinary Medicine in 2013. He graduated with a certificate in...